Acute necrotizing ulcerative gingivitis also known as ANUG. It is a common condition seen in my daily OPD. When there is a foul breath from the patient, as a dentist we used to suspect a case of ANUG. They are commonly seen in patients who smoke and have stress. It can also be due to many other causes which I will be talking about but these two are the main causes.
Contents
WHAT DO YOU MEAN BY ANUG?
From the term itself will come to know that it’s an infection that affects our gingiva. In other words, it can also be defined as it’s an endogenous [means having an internal origin] infection which is characterized by necrosis of the gingival or gums.
Acute necrotizing ulcerative gingivitis is known by different names such as
- Trench mouth
- Vincent’s gingivitis
- Vincent’s gingivostomatitis
- Pseudomembranous angina
- Fusospirochetal gingivitis
- Ulceromembranous gingivitis
When I was preparing for my NEET MDS ANUG was one of the important topics from Periodontology and in most of the MCQs they use the term Vincent’s gingivitis instead of ANUG.
WHAT IS THE ETIOLOGY?
The main etiology is:
- Smoking.
- Stress.
- Poor oral Hygiene.
It can also be due to any injury to the gingiva or any trauma to the gingiva.
If the patient comes to you with gingival diseases or gingivitis it can give a clue that it is ANUG. The two bacteria which affect are fusiform bacillus and Spirocheal organism also known as Borellia Vincenti. Fusiform bacillus from the term itself will come to know that it is rod-shaped having one blunt end and the other pointed.
The other factors are systemic factors such as:
- Nutritional deficiency mainly vitamin C.
- Deficiency of vitamin B2 [Riboflavin].
Riboflavin is an essential vitamin needed in our body, they are necessary for normal cell growth and function. They are found in food such as milk, meat, eggs, nuts, green vegetables, etc.
Acute necrotizing ulcerative gingivitis is also seen in patients with cancer, syphilis, and severe gastrointestinal disorders. In most of the cases, HIV-positive cases show ANUG.
As I mentioned earlier mental stress can also cause ANUG.
WHAT ARE THE SYMPTOMS?
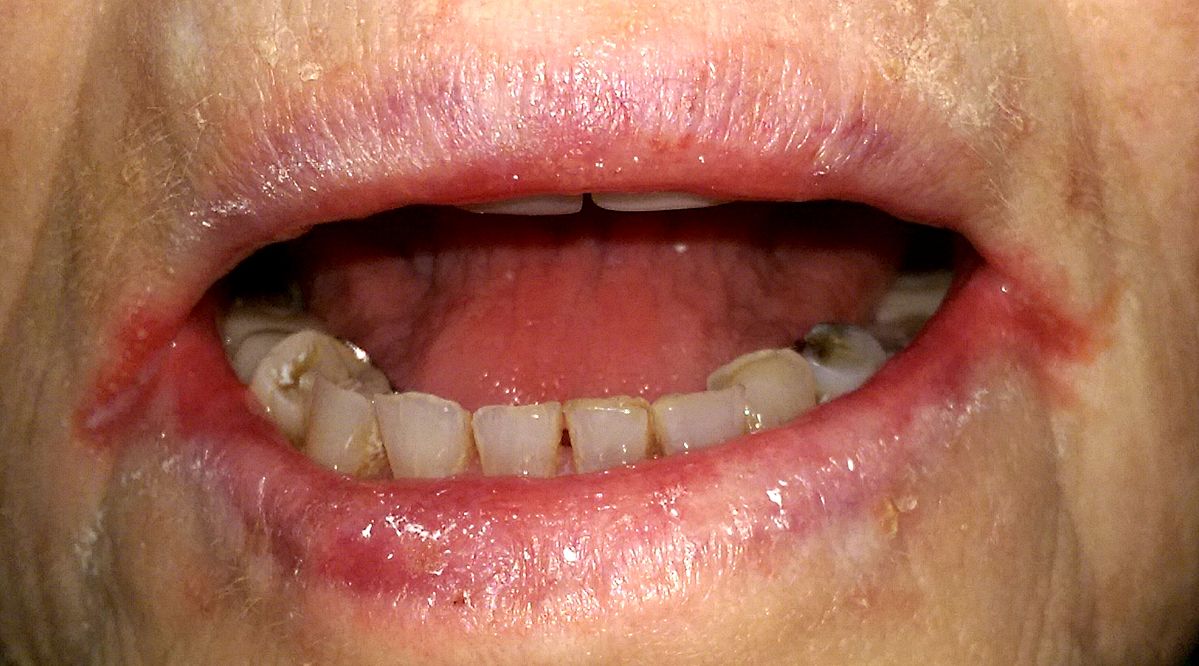
The first symptom is an unpleasant odor. A patient comes to you complaining of an unpleasant odor or bad breath. He complains of excessive bleeding while brushing from the gums or gingiva.
The patient complains of severe pain and tenderness. Profuse or abundant salivation having pasty saliva. The patient always complains of a metallic taste. Pain is always radiating with worrying or distressing pain. The pain always aggravates while having spicy and hot foods.
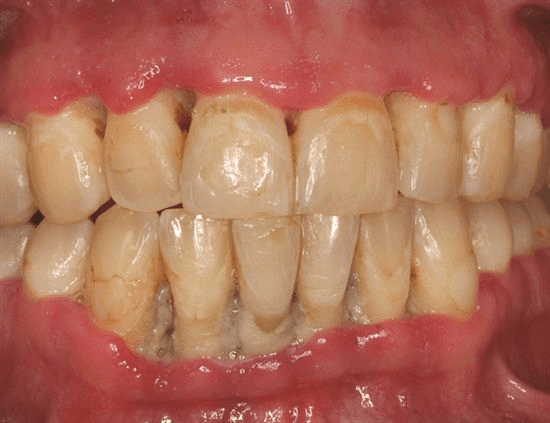
Intra-oral examination shows blunting [becomes less sharp] of interdental papilla. The color of the gingival becomes brown in color.
Some of the tooth becomes extruded from the socket and the patient always complains of sensitivity. Localized recession is present. Recession is a condition of exposure of roots of the teeth due to loss of gum tissue. Extrusion of teeth from the socket causes mobility of teeth which results in difficulty while having food.
The intra-oral examination shows punched-out crater-like ulceration on the gingiva. Punched-out crater-like ulceration should always be kept in mind when we talk about ANUG.
Ulceration of the gingival is another irritating clinical feature.
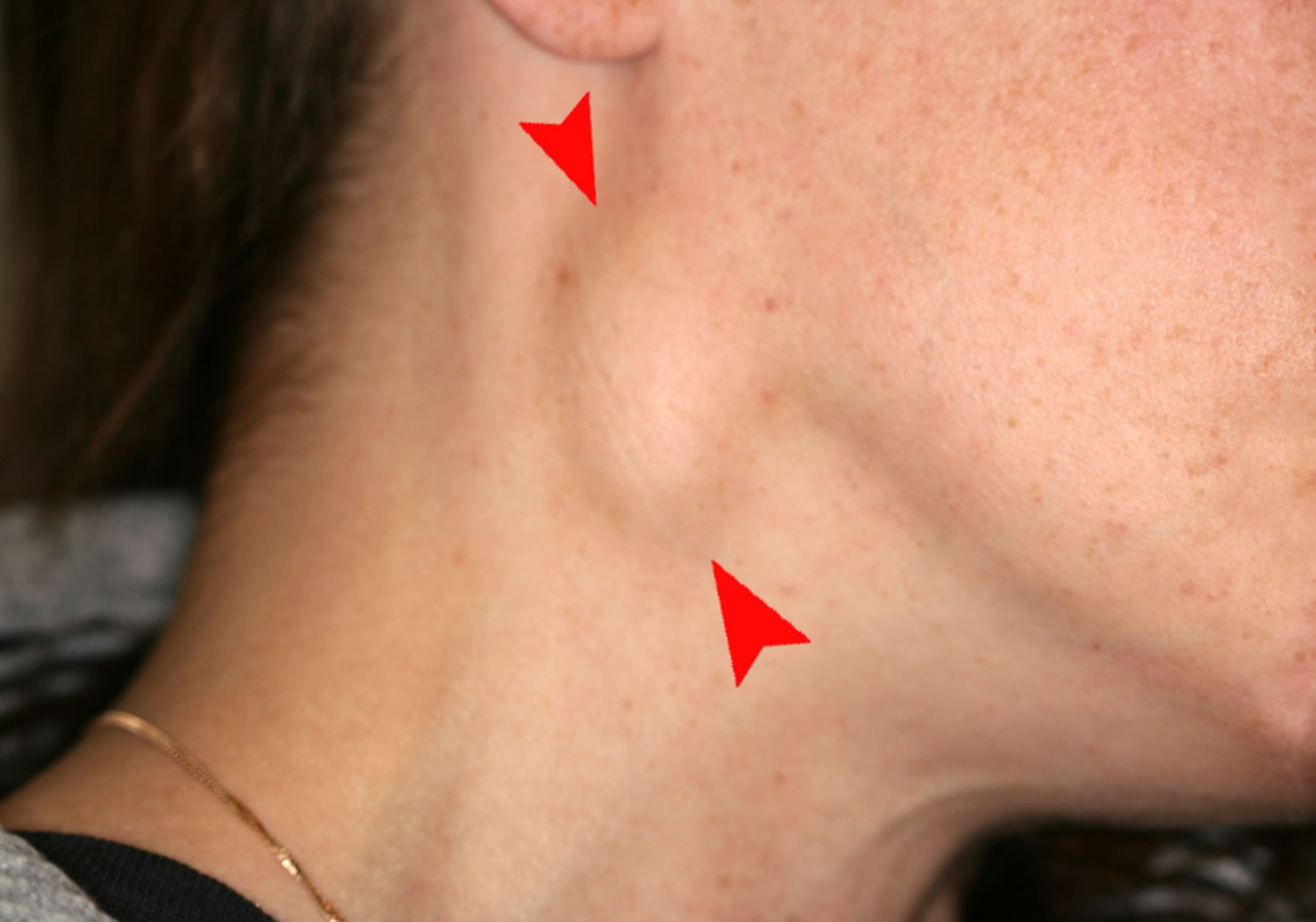
Due to all the above factors, the patient experiences high fever, increased pulse rate, and decreased appetite which is a lack of intake of food. The intraoral and extra-oral lymph node examination shows a regional lymphadenopathy.
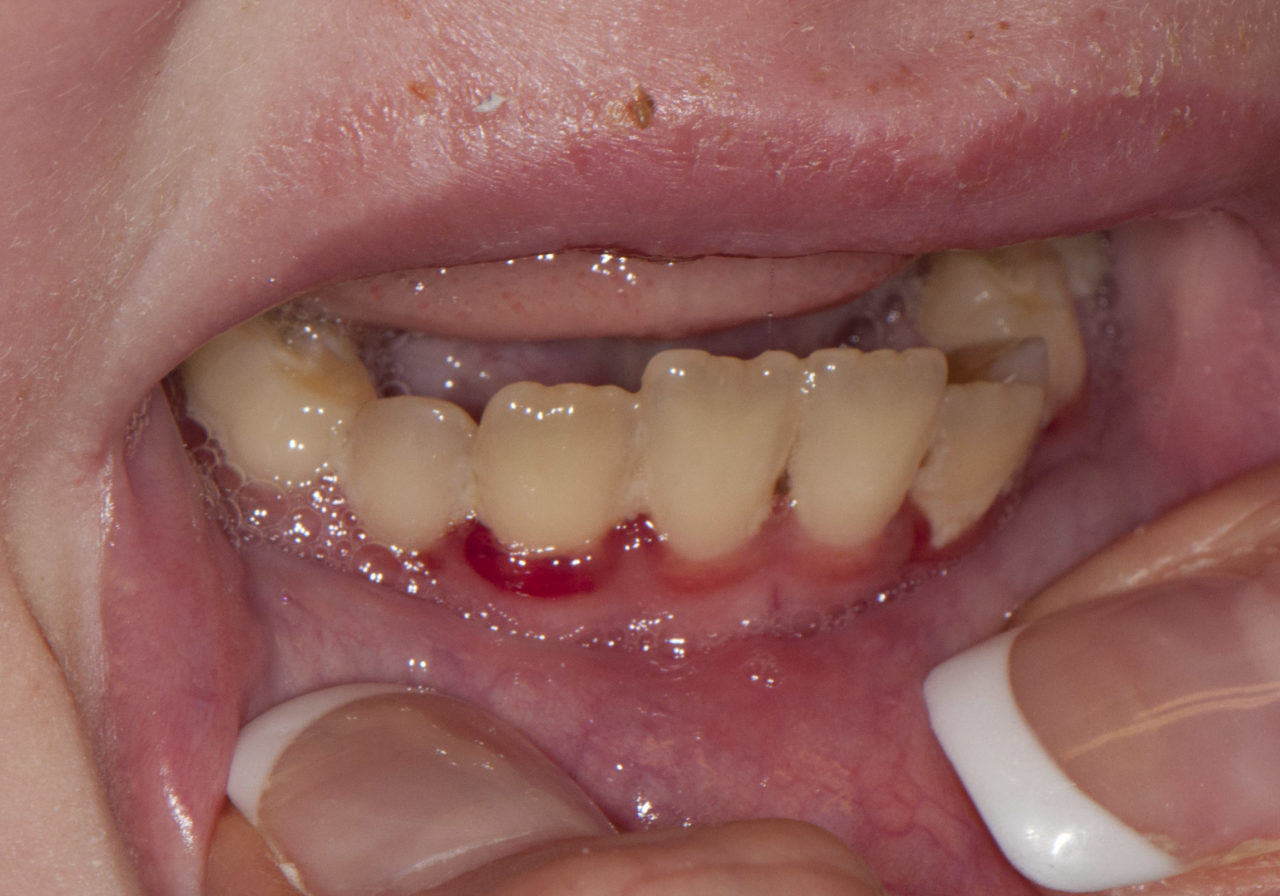
(A) Typical punched-out papilla between the mandibular canine and lateral incisor is covered by a grayish-white pseudo membrane.
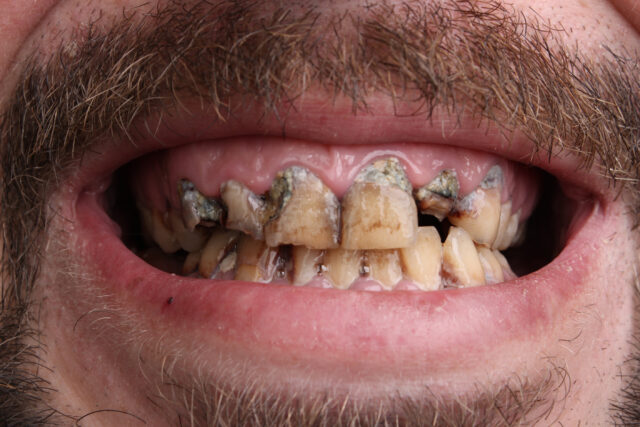
(B) More advanced case shows the destruction of the papillae, which results in an irregular marginal contour.
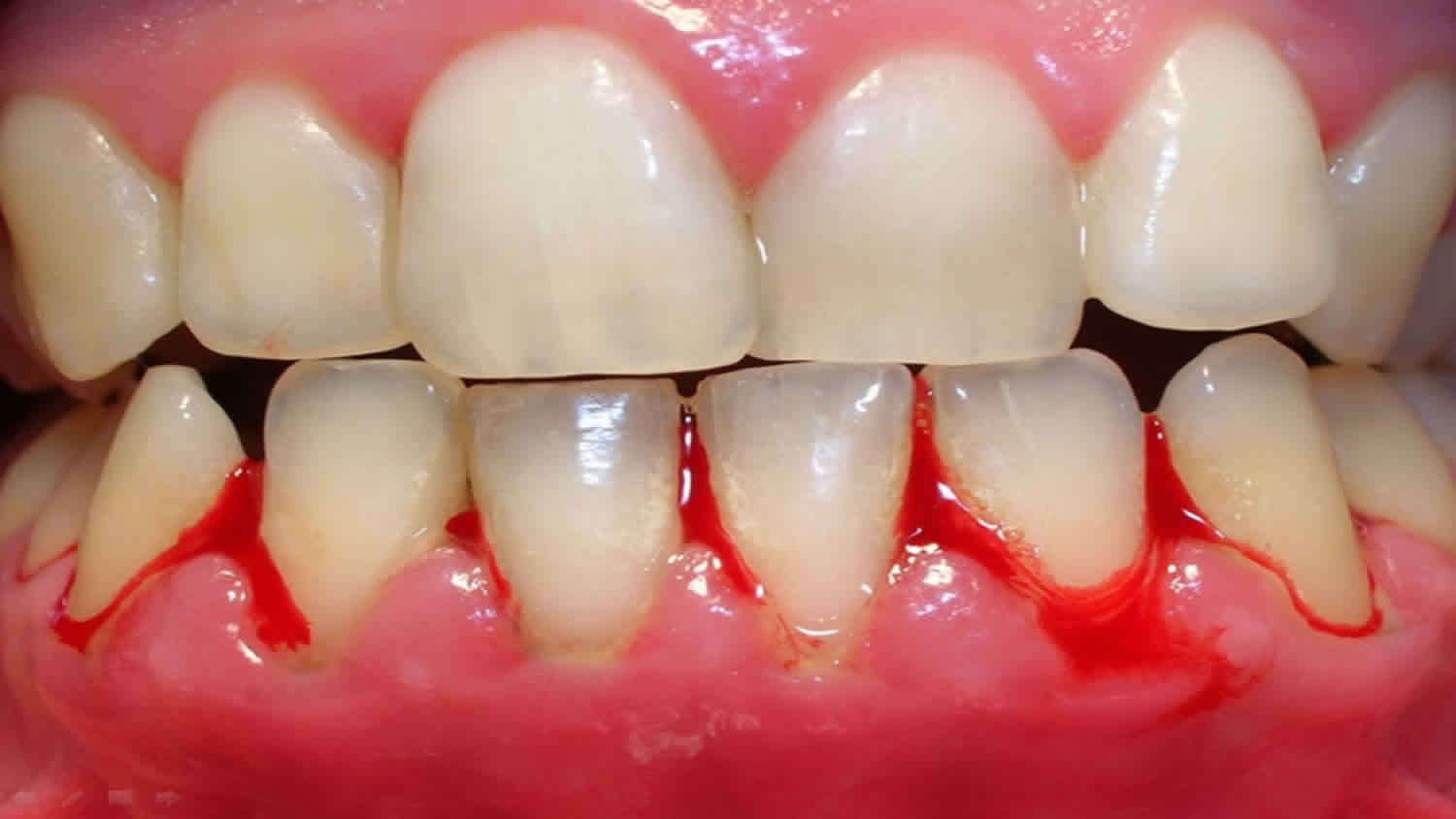
(C) Typical lesions with spontaneous hemorrhage.
(D) Generalized involvement of the papillae and the marginal gingiva with whitish necrotic lesions.
WHAT ARE THE COMPLICATIONS OF ANUG?
The systemic complications include fever as we discussed above, and lymphadenopathy in the earlier stages.
In the later stages the fever becomes high, increased WBC count. An increase in WBC in any case indicates infection.
If the ANUG is not treated well in the initial stages it leads to ANUP which is acute necrotizing ulcerating periodontitis that is it affects the periodontium.
HOW WILL YOU DIAGNOSE?
- The diagnosis is based on gingival pain, ulceration, and bleeding.
- Gingival pain is a radiating pain intensified by having spicy or hot food.
- A punched-out crater-like depression is seen in the gingival.
- Spontaneous bleeding on probing is present.
WHAT ARE THE DIFFERENTIAL DIAGNOSES?
The differential diagnosis includes agranulocytosis, which is a blood disorder characterized by a severe decrease in the amount of white blood cells. Vincent angina is a condition characterized by pain, swelling, and ulceration seen in the mouth and throat.
Gonococcal stomatitis is a sexually transmitted disease that mainly involves the mucous membrane and leads to urethritis, cervicitis, etc. Desquamative stomatitis is a condition with erythematous gingival and erosion of gingival epithelium.
HOW WILL YOU TREAT?
The treatment plan includes 2 steps:
- Treatment of non-ambulatory patients.
- Treatment of an ambulatory patient.
TREATMENT FOR NON-AMBULATORY PATIENT.
Nonambulatory means a patient who is unable to walk but who may be mobile with the help of a chair or other mobile devices.
- First day with the help of a cotton pellet gently remove the pseudo membrane.
- The patient is advised to gently rinse their mouth every 2 hours with diluted 3 percent hydrogen peroxide.
- First-day local treatments are restricted.
- The patient is advanced to have penicillin or metronidazole.
- Proper bed rest is advised.
- On the second day if the condition improves better will move to the next step which is the periodontal procedure. But if there is no improvement in the patient at the end of 24 hours will wait for a few more days and be advised for bed rest. The treatment will be the same as mentioned on the first day which is rinse with 3 percent of hydrogen peroxide.
- On the third day if the condition is improved start the treatment for ambulatory patients.
TREATMENTS FOR AMBULATORY PATIENTS?
- On the first day topical local anesthesia is given and will wait for 5 minutes. With the help of a cotton pellet gently swab the affected area to remove the pseudo membrane and non-attached surface debris.
- With the help of warm water wash the area. Superficial calculus is removed with the help of ultrasonic scalers. Deep calculus and debris are not removed now due to infection and severe bleeding.
- If the patient is having severe ANUG and lymphadenopathy then advice for antibiotic therapy.
- Penicillin V 500mg, thrice a day for 7 days
- Metronidazole 400mg twice a day for 7 days
What are the instructions to the patient?
- Rinse with 3 percent hydrogen peroxide and warm water for every 2 hours
- Avoid smoking and alcohol.
- In the second visit scaling and curettage can be done. The gingiva looks shrank previously calculus can be exposed. Continue the same instruction mentioned above.
- In the third visit, scaling and root planning are repeated. The use of hydrogen peroxide is discontinued. Plaque control instructions are given.
- In the fourth visit thorough scaling and root planing were performed.
- In the fifth visit treatment for elimination of all local irritants, periodontal pockets, and periodontal flaps.
Other treatment
The patient is advised to have plenty of fluid intake. Advised to have a proper diet plan with balanced nutrient supplements. Bed rest is a must for patients with severe complications. The patient is advised to take water-soluble vitamins B and C.
Mouth rinsing
1. The patient is advised to take 0.12 percent chlorhexidine twice a day.
2. Mouth rinsing is a must every 2 hours with warm water and hydrogen peroxide.
ADVICE FOR THE PATIENTS
If the infection is not treated well it leads to acute necrotizing ulcerative periodontitis [as we discussed above], Noma, stomatitis, infections to the jaw, cheeks adjacent soft tissues, etc.
Proper treatment such as scaling, and root planning helps to prevent the disease to a serious condition.
So, I suggest everyone consult a dentist as soon as possible to prevent further complications.
Similar to ANUG there is a condition called Angular Cheilitis. I have written a detailed blog about the same. I have faced many questions related to that topic when i was preparing for my NEET examination.
I tried my best to include all the information about ANUG. If you feel I missed out something, then feel free to comment it below.
Even if you have any questions, you can comment below, and I will try my best to revert back as soon as possible.
One Small Request: If you think this article helped you in any way, then please do share it with your friends. This will help me build my readers, and it motivates me to write more and more content like this.